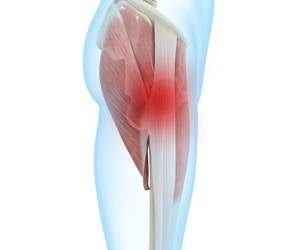
Articular cartilage tear


What is cartilage? Cartilage is a type of rubbery connective tissue that acts as a cushion between bones in joints. It is prone to damage and, because it lacks blood vessels and nerves, it takes much longer to heal compared to normal tissue. When joint cartilage, also known as articular cartilage, is damaged, it can cause severe pain, inflammation, and some degree of disability. This type of cartilage damage is most common in the knees, but other joints like the elbows, wrists, ankles, shoulders, and hips can also be affected.
What causes knee cartilage damage? Knee cartilage damage can occur due to trauma (such as an accident) or gradual degeneration (sometimes referred to as wear and tear). Certain activities are more likely to cause articular cartilage damage, including:
- High-intensity sports injuries: Direct impact on the joints can damage cartilage, which is common among people involved in high-intensity sports.
- Lack of exercise: Conversely, lack of exercise can also lead to cartilage damage, especially among “weekend warriors” who only engage in physical activities on weekends, making them more prone to sudden, intense movements. Joints need regular movement to stay healthy, and long periods of inactivity increase the risk of cartilage damage.
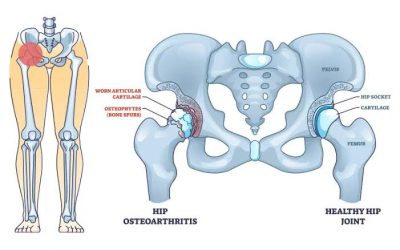
- Obesity and prolonged joint pressure: Prolonged pressure on joints can also cause cartilage damage, particularly in weight-bearing joints like the knees. People who are overweight or obese are especially at risk, and this long-term stress can eventually lead to cartilage breakdown, known as osteoarthritis.
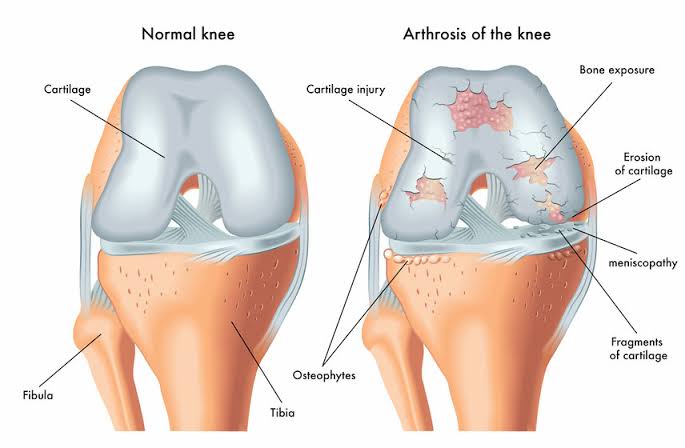
Symptoms of knee cartilage damage If you have knee cartilage damage, you might experience the following symptoms:
- Joint pain, even at rest, which worsens when bearing weight
- Swelling around the knee
- Stiffness in the knee
- Clicking or grinding sensation when moving
- Feeling like the knee is locking, getting stuck, or dislocating
How is knee cartilage damage diagnosed? The symptoms of sprains, ligament injuries, and cartilage damage are often similar, making them difficult to differentiate. However, non-invasive tests now make diagnosis easier than before. To confirm the source of the pain, doctors may order the following diagnostic tests:
- Magnetic Resonance Imaging (MRI): This uses magnetic fields and radio waves to create detailed images of the body, but it may not always detect cartilage damage.
- Arthroscopy: This involves inserting a tubular device called an arthroscope into the joint for examination. Arthroscopy helps assess the extent of cartilage damage.
How is knee cartilage damage treated? If your injury is not severe, non-surgical treatments like injections and supplements may be sufficient to treat your knee cartilage damage. Your doctor may recommend one of the following methods:
1.Injection Therapy: Many patients seek “miracle” injections, which may be simple cortisone injections (sometimes called H+L), designed to suppress inflammation and provide immediate pain relief. However, this is only a temporary fix and does not address the root cause.
2.Viscosupplementation: This treatment involves injecting a thick fluid called hyaluronic acid into the joint, often recommended for early-stage cartilage defects or minor injuries. Hyaluronic acid acts as a lubricant, allowing bones to move smoothly and serving as a shock absorber to reduce joint stress. The effectiveness diminishes over time, so these treatments are usually repeated every 6 to 12 months.
3.Platelet-Rich Plasma (PRP) Injection: In recent years, there has been much discussion about platelet-rich plasma (PRP) therapy, though its potential effects remain inconclusive. PRP involves injecting concentrated platelets, which contain proteins that promote healing, into the injured area. Some athletes like Tiger Woods and tennis star Rafael Nadal have used PRP therapy for various injuries.
4.Stem Cell Therapy: Stem cell therapy is often regarded as a cure-all, but apart from knee stem cell therapy, there’s limited scientific evidence supporting this claim. Stem cell therapy for knee osteoarthritis has shown promising results in reducing inflammation, alleviating pain, and repairing cartilage, helping many patients avoid surgery. However, the exact mechanisms by which stem cells work remain unclear, and more research is needed.
5.Surgical Treatments for Knee Cartilage Repair Surgery is typically reserved for severe cases where conservative treatments have failed. Depending on your age, activity level, the extent of the cartilage damage, and how long you’ve had the injury, several surgical options are available. It’s important to discuss with your doctor whether surgery is necessary and which type is best suited to treat your knee cartilage damage.
Surgical options include:
- Debridement: The surgeon smooths the damaged cartilage and removes loose edges to prevent cartilage from rubbing and irritating the joint.
- Microfracture: Small holes are drilled under the cartilage to expose blood vessels in the bone, triggering the formation of new cartilage. This new cartilage eventually matures into a durable repair tissue.
- Osteochondral Autograft Transplantation (OATS): Healthy, undamaged cartilage is taken from one area and transferred to the damaged area. This surgery is suitable for isolated areas of cartilage damage but not for widespread conditions like osteoarthritis.
- Autologous Chondrocyte Implantation (ACI): A small piece of cartilage is removed and sent to a lab, where more cartilage cells are cultured. After 1-3 months, the new cells are implanted into the joint.
- Knee Arthroscopy: A minimally invasive surgery where a tiny camera (arthroscope) is inserted into the knee joint, allowing the surgeon to view and correct problems.
- Cartilage Regeneration (MACI): This procedure uses cartilage-forming cells taken from the body and implanted in the damaged area through surgery to restore cartilage.
Though cartilage cannot heal on its own, there are numerous treatment options available. Depending on the severity of the damage, both non-surgical and surgical treatments can help manage your injury. Always consult with a doctor to determine the best course of action for your specific case.