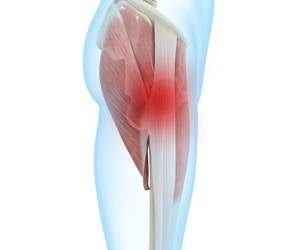
Dysmenorrhea
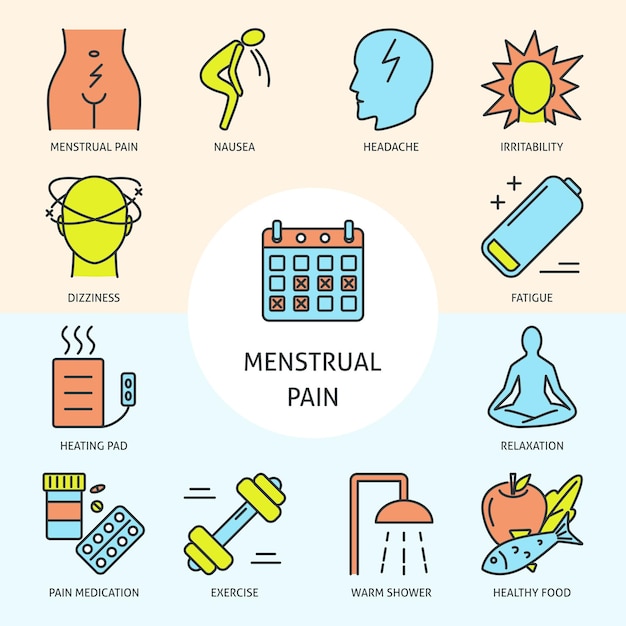
Dysmenorrhea Causes During menstruation, the uterus contracts to help shed the endometrium. Hormonal substances (prostaglandins) associated with pain and inflammation trigger uterine muscle contractions. Elevated prostaglandin levels can cause more severe dysmenorrhea.
Dysmenorrhea can be caused by the following reasons:
• Endometriosis: Tissue similar to the lining of the uterus begins to grow outside the uterus, most commonly in the fallopian tubes, ovaries, or pelvic peritoneum.
• Uterine fibroids: These noncancerous growths in the uterine wall can cause pain. • Adenomyosis: Tissue from the lining of the uterus begins to grow and infiltrate the muscle wall of the uterus.
• Pelvic inflammatory disease: This infection of the female reproductive organs is usually caused by sexually transmitted bacteria.
• Cervical stenosis: Some women may have narrow cervical openings, leading to poor menstrual flow and increased pressure within the uterus, resulting in dysmenorrhea.
• Nonsteroidal anti-inflammatory drugs (NSAIDs)
• Hormonal contraceptives are commonly used.
• Treatment of underlying conditions.
If dysmenorrhea is caused by other underlying conditions, targeted treatment should be pursued if possible. For example, cervical stenosis can be temporarily relieved by surgically widening the narrow cervix. If necessary, surgical removal of uterine fibroids or ectopic endometrial tissue (caused by endometriosis) can be performed.
If women with primary dysmenorrhea do not have a specific treatable condition, they can use general measures or take NSAIDs to relieve symptoms.
Treatment for Dysmenorrhea General measures Applying heat to the abdomen can also be helpful. Ensuring adequate sleep and rest, and engaging in regular exercise may also be beneficial. Other measures that may help alleviate pain include a low-fat diet and supplements such as omega-3 fatty acids, flaxseed, magnesium, vitamin B1, vitamin E, and zinc. There is not much evidence to support the usefulness of diet or these nutritional supplements, but most carry a low risk, so some women may consider trying them. Women should consult with their doctor before using these supplements.
Medications If the pain is bothersome, taking nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen, naproxen, or mefenamic acid may help. NSAIDs should be taken 24 to 48 hours before menstruation starts and continued for one to two days after menstruation begins.
If NSAIDs are ineffective, the doctor may also recommend contraceptive pills containing synthetic forms of the hormone progesterone (progestin) and estrogen. These medications prevent the ovaries from releasing eggs (ovulation). Women who cannot take estrogen can take progestin-only contraceptive pills.
If NSAIDs or contraceptive pills do not alleviate symptoms, other hormone treatments can be used. These include progestin (such as oral levonorgestrel, norethindrone, medroxyprogesterone, or micronized progesterone), gonadotropin-releasing hormone (GnRH) agonists (such as leuprorelin and nafarelin), GnRH antagonists (such as elagolix), and release of progesterone-releasing IUD or danazol (a synthetic androgen). GnRH agonists and antagonists help relieve dysmenorrhea caused by endometriosis. Danazol is not commonly used due to its many side effects.
Other treatments If a woman is suspected of having endometriosis, medication is ineffective, or infertility is present, the doctor may perform laparoscopic surgery to confirm the diagnosis of endometriosis and remove endometrial tissue located outside the uterus (endometrial implants).
If severe pain persists after various types of treatments, the doctor may perform a surgery to block uterine nerves, thereby blocking pain signals. These surgeries include: • Nerve injections with anesthetics (nerve blocks) • Destruction of nerves with laser, electricity, or ultrasound • Nerve ablation Nerve-blocking surgeries can be performed using laparoscopy. Occasionally, other organs in the pelvic cavity, such as the ureters, may be damaged when these nerves are severed.
Several alternative therapies have been proposed for the treatment of dysmenorrhea but have not been well-studied. These include behavioral counseling (such as systematic desensitization and relaxation, as well as pain management training), acupuncture, and acupressure. Hypnosis has also been demonstrated as an effective treatment method through research.