Hip Osteoarthritis
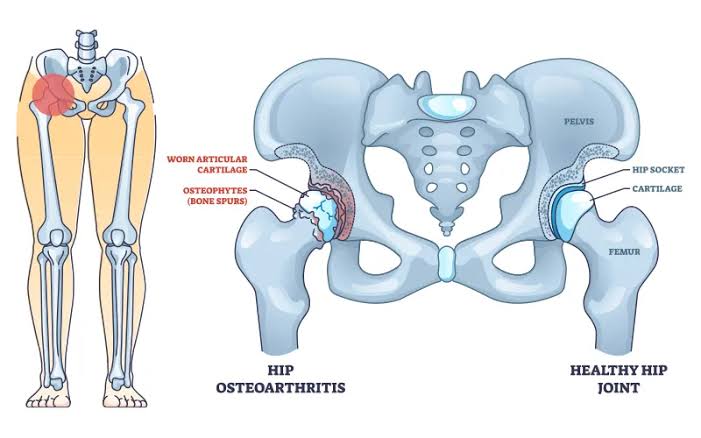

Hip osteoarthritis typically refers to a type of osteoarthritis caused by long-term uneven weight-bearing on the hip joint, leading to degeneration of the joint cartilage or structural changes in the bone. Its main symptoms include pain in areas such as the outer hip, groin (which may radiate to the knee), swelling, joint effusion, cartilage wear, bone spur formation, joint deformity, restricted internal rotation and extension of the hip, difficulty walking, and even being bedridden in severe cases.
Causes:
The exact cause is unclear, but it is generally believed to be related to aging, trauma, inflammation, obesity, and metabolic factors.
1.Obesity
There is a proportional relationship between increased body weight and the incidence of hip osteoarthritis. Obesity is a factor that exacerbates the condition. Weight loss in obese individuals can reduce the incidence of hip osteoarthritis.
2.Cartilage Structure
When cartilage becomes thinner and stiffer, its ability to withstand pressure decreases, increasing the likelihood of hip osteoarthritis.
3.Trauma and Physical Stress
When the joint is subjected to muscle imbalance and localized pressure, degenerative changes in the cartilage occur. Healthy joints and normal activities, even after strenuous exercise, generally do not lead to osteoarthritis.
4.Genetic Factors
Genetic influences on osteoarthritis may include congenital structural abnormalities and defects (e.g., congenital hip dislocation, femoral head epiphysis dislocation), cartilage or bone metabolism abnormalities, obesity, and osteoporosis.
Clinical Manifestations
The onset is insidious and progresses slowly, often seen in middle-aged and elderly individuals with a history of long-term overuse. The main symptoms include gait abnormalities and hip pain when active or bearing weight. Hip pain can radiate through the obturator nerve to the groin, thigh, and knee. There may also be a dull aching sensation around the buttocks and greater trochanter, radiating to the lateral and posterior thigh.
Examination
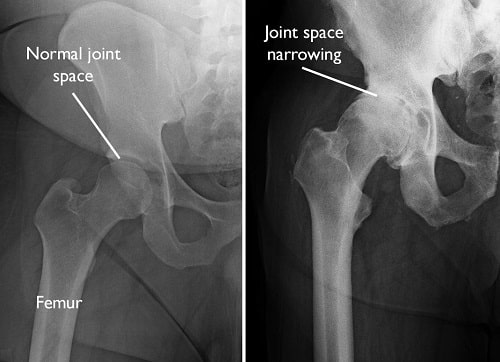
- Repeated hip joint pain over the past month.
- X-ray shows osteophyte formation, acetabular rim hypertrophy, and joint space narrowing in the hip.
Treatment
1.General Treatment
This includes patient education, self-training, weight loss, aerobic exercises, joint mobility training, muscle strength training, the use of walking aids, valgus knee wedge insoles, occupational therapy, joint protection, and assistive devices for daily living.
2.Medication
(1) Hyaluronic Acid: A main component of synovial fluid in joints and a part of the cartilage matrix, it provides lubrication and reduces friction between tissues. Injecting it into the joint cavity can significantly improve inflammation in synovial tissues, enhance the viscosity and lubricating function of joint fluid, protect cartilage, relieve pain, and increase joint mobility. It is typically injected into the joint at a dose of 25 mg once a week for five weeks, with strict aseptic procedures required.
(2) Glucosamine: An important monosaccharide in glycosaminoglycans and proteoglycans, essential components of joint cartilage matrix. In osteoarthritis, cartilage cells’ ability to synthesize glycosaminoglycans is impaired or insufficient, leading to cartilage matrix softening, loss of elasticity, collagen fiber destruction, and increased bone wear and damage. Glucosamine sulfate blocks the mechanisms of osteoarthritis, promotes the synthesis of proteoglycans with a normal structure, inhibits the production of enzymes that damage tissue and cartilage (e.g., collagenase, phospholipase A2), reduces cartilage cell damage, improves joint mobility, alleviates joint pain, and slows the progression of osteoarthritis. The recommended daily dose is 1500 mg, taken with meals.
(3) Non-Steroidal Anti-Inflammatory Drugs (NSAIDs): These drugs inhibit cyclooxygenase and prostaglandin synthesis, counteracting inflammation, reducing joint swelling, and relieving pain. Options include ibuprofen, glucosamine and zinc, or nimesulide.
Surgical Treatment
When symptoms of hip osteoarthritis are severe, unresponsive to medication, and interfere with daily life, surgery should be considered. However, joint replacement surgery carries short- and long-term complications, such as component loosening, wear, and bone resorption, which have yet to be fully resolved. The outcome of artificial joint replacement is closely related to the length of the surgery, the surgeon’s experience, the patient’s preoperative condition, perioperative management, and rehabilitation training. Thus, artificial joint replacement should be approached cautiously.
Prognosis
It is recommended to get ample sunlight, stay warm, and avoid cold and damp conditions to give the hip joint proper rest. Once the pain is relieved, walking on flat surfaces for 20-30 minutes a day is beneficial. Try to minimize activities that stress the joint, such as going up and down stairs, bending over, and running, to prevent further cartilage wear and tear.