What is Achilles tendinitis?
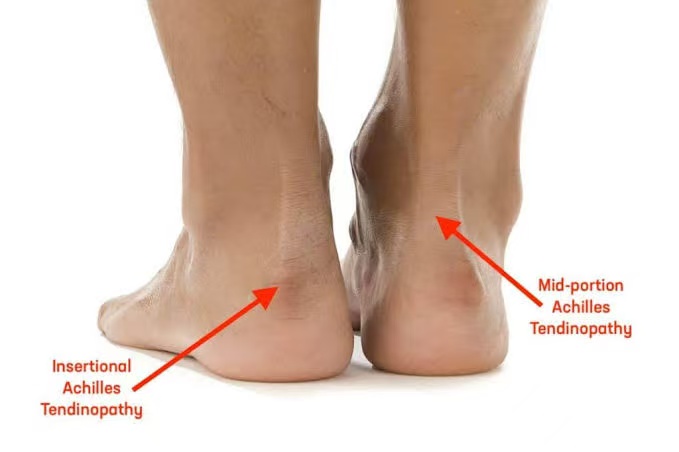

Achilles tendinitis refers to Achilles tendon injury.
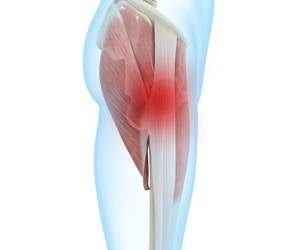
The Achilles tendon is located at the back of the ankle, connecting the calf muscles (gastrocnemius) to the heel bone (calcaneus). It is the largest tendon in the human body and is essential for walking, running, and jumping. This tendon bears significant pressure during daily activities.
When the muscles and Achilles tendon are overused, it can cause tendon irritation and swelling, leading to Achilles tendinitis.
Types of Achilles tendinitis
- Insertional Achilles tendinitis
- Affects the lower part of the tendon where it attaches to the heel.
- Can occur at any age.
- Non-insertional Achilles tendinitis
- Affects the middle portion of the tendon, causing swelling and thickening.
- More common in younger people and those who are physically active.
Both types of Achilles tendinitis may lead to tendon fiber hardening (calcification) in the damaged area.
What are the symptoms of Achilles tendinitis?
If you have Achilles tendinitis, you may experience heel pain and swelling at the back of the heel.
Consult a doctor if you experience:
- Inability to bend your ankle
- Difficulty walking comfortably on the affected side
- Calf swelling
- Joint deformity due to injury
- Ankle pain during rest or at night
- Persistent ankle pain for several days
- Signs of infection, such as warmth, redness, or heat in the heel area
What causes Achilles tendinitis?
Achilles tendinitis is usually caused by:
- Overuse or repetitive stress on the tendon (small repetitive impacts)
- Sudden injury
What are the risk factors for Achilles tendinitis?
Risk factors for Achilles tendinitis include:
- Age: Older adults are more likely to develop Achilles tendinitis.
- Bone spurs: Heel bone spurs can irritate the Achilles tendon, causing pain and swelling. The likelihood of developing bone spurs increases with age.
- Gender: Achilles tendinitis is more common in men.
- High-intensity activities: Sports involving jumping and landing (e.g., basketball) or running on hard surfaces increase the risk of tendon damage.
- Excessive activity: Running too much, sudden increases in activity, or running uphill can strain the tendon.
- Certain medical conditions: Conditions like psoriasis or hypertension increase the risk of Achilles tendinitis.
- Medication use: Fluoroquinolone antibiotics are associated with a higher incidence of Achilles tendinitis.
- Obesity: Excess body weight puts extra stress on the Achilles tendon.
- Body structure: Flat feet place additional strain on the tendon.
- Inadequate warm-up: Tight calf muscles without proper stretching can strain the Achilles tendon.
- Worn-out shoes: Insufficient support from old shoes can lead to tendon strain.
What are the complications and related conditions of Achilles tendinitis?
Achilles tendinitis may lead to Achilles tendon rupture, which is a partial or complete tear of the tendon. This condition typically causes severe pain and may require surgical intervention.
Possible complications from surgery include:
- Nerve damage
- Delayed healing
- Weakness in the calf
- Persistent or recurring pain in the foot and ankle
Your age, overall health, and the condition of your foot and leg muscles may also affect your surgical risks and outcomes. Consult your doctor for personalized information on risks and recommended treatments.
How can Achilles tendinitis be prevented?
To reduce the risk of heel pain and Achilles tendon injury, follow these preventive measures:
- Alternate activities: Switch between high-impact (e.g., running, basketball) and low-impact (e.g., swimming, cycling) exercises to prevent overuse.
- Gradually increase intensity: When starting a new sport or exercise program, begin slowly and increase intensity gradually.
- Modify workouts: Avoid activities that excessively strain the tendon, such as uphill running. Stop if you feel pain.
- Daily stretching: Stretch frequently—not just before and after exercise—to maintain calf muscle flexibility.
- Strengthen calf muscles: This helps the Achilles tendon withstand daily stress and physical activity.
- Warm up thoroughly: Stretch properly, especially before strenuous activities.
- Wear supportive shoes: Choose shoes with good arch support and cushioning, or use orthotic insoles like arch supports to reduce stress on the tendon.